Ethical practice in therapy does not break down in obvious ways. It usually shows up in small decisions you make every day, what you document, what you choose not to say, how you respond when a client shares something that sits in a grey area.
You are not just following guidelines. You are applying judgment in situations where confidentiality, client autonomy, and legal responsibility do not always align perfectly.
In 2026, these decisions have become more layered. You may be working across in-person and digital sessions, handling sensitive data across platforms, or navigating boundaries that extend beyond the therapy room into messaging, scheduling, and online presence. The rules themselves have not changed significantly, but the contexts in which you apply them have.
This guide brings together 15 core therapist rules, not as a checklist, but as a practical reference for how you apply them in real situations. The focus is on consistency, defensibility, and maintaining clinical integrity as your practice evolves.
Key Takeaways
- Therapist rules form the foundation of ethical, safe, and legally compliant practice, guiding every aspect of client interaction and care.
- Confidentiality remains critical, but therapists must also understand when and how to apply its limits in complex, real-world situations.
- Professional boundaries are not static—they require ongoing awareness and adjustment, especially in long-term or digital therapy settings.
- Ethical practice involves more than following guidelines; it requires clinical judgment, self-reflection, and consistency across cases.
- In 2026, factors like teletherapy, data privacy, and social media have made applying these rules more nuanced and demanding.
- Proper documentation and secure systems are essential for maintaining compliance, continuity of care, and defensible decision-making.
- Platforms like Simply.Coach help therapists manage records, consent, and communication in a structured way, supporting ethical and consistent practice.
What Are Therapist Ethical Rules and Why They Matter in 2026
Therapist ethical rules are not something you refer to occasionally. You apply them continuously, often in situations where there is no clearly defined “correct” response. Most ethical decisions in practice do not come from obvious violations.
They emerge in moments where confidentiality, client autonomy, and legal responsibility intersect, and you are required to decide in real time how to proceed.
In day-to-day work, this shows up in how you interpret disclosures, manage boundaries as relationships evolve, and document sessions that may later require justification. These are not isolated actions. They are connected decisions that shape the safety, clarity, and defensibility of your practice over time.
Where these rules show up in your clinical work
You are not applying ethical frameworks in abstraction. You are applying them inside specific situations that develop gradually and often without clear thresholds.
- Risk-related disclosures: You are assessing intent, immediacy, and context while deciding whether confidentiality still holds or needs to be limited.
- Boundary shifts over time: Familiarity, informal communication, or small deviations in structure can accumulate. The challenge is identifying boundary drift early, not after it becomes a violation.
- Session documentation: You are deciding what is clinically relevant, what may need to be referenced later, and how to document sensitive material without overexposure.
- Digital interactions and tools: Whether it is video, messaging, or record systems, you remain responsible for how client data is handled across each point of contact.
Each of these requires judgment that cannot be reduced to a rule. The rule provides direction, but the application depends on context.
Why applying these rules is more complex in 2026
The principles themselves have remained stable, but the conditions under which you apply them have changed. Therapy is no longer confined to a controlled, in-person setting. Communication extends beyond sessions, and records are stored and accessed across multiple systems.
At the same time, clients are more aware of privacy, consent, and data handling. This increases the need for clarity, both in how you work and how you explain your decisions.
Key shifts affecting practice:
- Hybrid and teletherapy delivery: You are managing confidentiality across environments you do not fully control.
- Higher expectations around data privacy: Clients are more likely to question storage, access, and usage of their information.
- Cross-context practice: Working across formats or locations introduces overlapping ethical and legal considerations.
- Technology in clinical workflows: Tools support your work, but responsibility for accuracy and confidentiality remains with you.
What this means for how you apply ethical rules
The challenge is not understanding ethical frameworks. It is applying them consistently when information is incomplete and outcomes are uncertain.
In practice, this means:
- assessing risk before acting, rather than reacting to urgency
- choosing the least intrusive intervention that still addresses the situation
- documenting not just what you did, but why you did it
- revisiting decisions when new information changes the context
Consistency becomes more important than individual decisions. Ethical practice is evaluated over time, across patterns, not isolated actions.
Where experienced therapists still encounter friction
Even with experience, certain gaps tend to appear. These are rarely due to lack of knowledge and more often due to assumptions or habit.
- Relying on past decisions without reassessing context: Similar situations can differ in small but important ways.
- Treating digital practice like in-person work: This often overlooks how confidentiality and boundaries shift in online environments.
- Documenting outcomes without reasoning: Decisions may be sound, but without rationale, they are harder to defend.
- Assuming tools ensure compliance: Platforms support structure, but they do not replace clinical judgment.
The shift in modern therapy practice
Ethical practice now requires active interpretation rather than passive adherence. You are applying established principles across changing contexts, adapting them to individual clients, and ensuring that your decisions remain consistent and defensible.
If you can clearly explain what you did, why you did it, and how it aligns with both clinical and legal expectations, your ethical framework is functioning as it should.
Also Read: 50+ Resources, Tools, and Worksheets for Therapists
Therapist Confidentiality Rules in Practice: How to Apply Them in Real Situations
Confidentiality is one of the few rules that directly shapes how much a client is willing to share with you. In practice, maintaining confidentiality is not just about protecting information. It is about making consistent decisions on when to hold, when to clarify, and when disclosure may be required.
For experienced therapists, the complexity is rarely in understanding the rule. It is in applying it when situations are not clearly defined, especially when risk, consent, and legal obligations overlap.
Where confidentiality decisions become less straightforward
Confidentiality is not tested in routine sessions. It is tested in situations where the boundaries of the rule are unclear.
- When a client shares something that may indicate risk: You are deciding whether the threshold for breaking confidentiality has been met, not just whether risk exists.
- When working with third parties (family, institutions, referrals): You are managing what can be shared, what should be shared, and what requires explicit consent.
- When handling digital communication: Messages, emails, and platform-based interactions introduce additional exposure points beyond the session.
- When documenting sensitive disclosures: You are balancing clinical accuracy with the risk of over-documenting information that may later be accessed.
These situations require interpretation, not just adherence.
Core confidentiality rules (and how to apply them correctly)
These rules are foundational, but their application depends on how you interpret context and risk.
1. Protect client confidentiality consistently: This includes verbal disclosures, written notes, and any identifying information across systems. In practice, this means:
- avoiding casual disclosures, even in professional settings
- ensuring conversations cannot be overheard in physical or digital environments
- being aware of indirect identifiers when discussing cases
2. Obtain informed consent before sharing information: Consent is not a one-time form. It is an ongoing understanding of how information may be used. In practice, this means:
- explaining limits of confidentiality clearly at the start
- revisiting consent when context changes (e.g., involving a third party)
- checking client understanding, not just obtaining agreement
3. Secure all client records and notes: Confidentiality extends to how information is stored, accessed, and transferred. In practice, this means:
- using secure, access-controlled systems
- avoiding storing sensitive data across multiple untracked locations
- ensuring only relevant individuals have access
4. Maintain confidentiality in digital communication: Digital interactions increase the number of points where confidentiality can be compromised. In practice, this means:
- using encrypted and privacy-compliant tools
- setting clear boundaries on communication channels
- avoiding sharing sensitive information over unsecured platforms
5. Apply the minimum necessary disclosure principle: When disclosure is required, the scope should be limited. In practice, this means:
- sharing only what is necessary for the specific purpose
- avoiding full case disclosures when partial information is sufficient
- documenting what was shared and why
Where experienced therapists need to be more deliberate
Confidentiality rarely breaks in obvious ways. It weakens through small, repeated decisions. Common patterns include:
- becoming less precise in informal discussions with peers
- over-documenting sensitive material without clear purpose
- assuming digital tools are secure without verifying settings
- not revisiting consent as the therapeutic context evolves
What strong confidentiality practice looks like
A well-applied confidentiality framework allows you to:
- make disclosure decisions without hesitation or guesswork
- explain your reasoning clearly if questioned
- maintain client trust even when limits need to be applied
- ensure records remain both clinically useful and appropriately protected
If you are consistently evaluating risk, documenting your reasoning, and limiting disclosure appropriately, your confidentiality practices are aligned.
Also Read:Top 18 Apps for Therapists to Use With Clients in 2026
Therapist Boundary Rules in Practice: How to Manage Boundaries with Clients
Boundaries are not tested in clear violations. They are tested in small shifts that feel reasonable in the moment but change the structure of the relationship over time.
In practice, boundary management is less about saying no to obvious issues and more about noticing when the frame of therapy begins to loosen. This is especially relevant in long-term work, small communities, or digital settings where access and familiarity increase.
The challenge is not identifying extreme cases. It is recognizing early changes before they affect objectivity, role clarity, or client dependence.
Where boundary issues typically begin
Boundary violations rarely start as violations. They begin as adjustments that seem clinically justified.
- Increased informality over time: Sessions may become less structured, communication more casual, or expectations less clearly defined.
- Extended access outside sessions: Messaging, check-ins, or availability may gradually expand beyond what was originally agreed.
- Subtle role shifts: You may find yourself moving between therapist, advisor, or support figure in ways that are not clearly defined.
- Unclear expectations in digital settings: Online therapy often blurs timing, availability, and communication norms.
These are not immediate problems, but they require attention before they become patterns.
Core boundary rules (and how they apply in practice)
These rules are well-known, but their application depends on how early you identify boundary movement.
1. Avoid dual relationships that affect objectivity: Dual roles are not always avoidable, especially in smaller communities. The issue is whether they interfere with your ability to remain clinically objective. In practice, this means:
- assessing whether the second role changes decision-making or power dynamics
- setting clear limits if some overlap cannot be avoided
- documenting the reasoning behind continuing or declining the relationship
2. Maintain clear therapeutic roles at all times: The therapeutic relationship depends on role clarity, even when rapport is strong. In practice, this means:
- keeping interactions focused on the client’s therapeutic goals
- avoiding over-involvement or taking on non-clinical roles
- monitoring when conversations shift away from therapeutic intent
3. Avoid romantic or sexual involvement without exception: This is a strict boundary, but the risk often lies in early signals rather than explicit actions. In practice, this means:
- noticing changes in tone, attachment, or dependency
- addressing transference or countertransference early
- maintaining clear distance even after termination, in line with ethical guidelines
4. Manage social media and digital boundaries actively: Digital presence creates ongoing exposure outside sessions. In practice, this means:
- not engaging with clients on personal platforms
- setting clear policies around communication channels
- being aware of how your online presence may affect the therapeutic dynamic
5. Recognize and address boundary drift early: Boundary issues rarely appear suddenly. They accumulate through small, repeated adjustments. In practice, this means:
- noticing increased informality or flexibility
- addressing shifts directly in session
- resetting expectations before patterns form
What boundary management looks like in ongoing work
In longer-term therapy, boundaries require continuous adjustment rather than one-time definition.
- revisit expectations around communication and availability
- check whether session structure is still consistent
- monitor dependency versus therapeutic progress
- address small shifts directly instead of waiting for escalation
The goal is not rigidity. It is maintaining a frame that supports the work.
Where experienced therapists still encounter difficulty
Boundary challenges often come from familiarity rather than lack of knowledge.
- allowing small exceptions that gradually become norms
- delaying conversations about boundary shifts to avoid discomfort
- underestimating how digital access changes expectations
- assuming strong rapport justifies flexibility
These patterns are subtle but cumulative.
What strong boundary practice looks like
When boundaries are well managed:
- roles remain clear even in long-term relationships
- communication stays consistent and predictable
- clients understand the structure of the work
- decisions remain clinically grounded rather than relationally driven
If you are identifying shifts early, addressing them directly, and maintaining consistency over time, your boundary framework is working.
Also Read:Best Mental Health Software for 2026: Top Platforms Compared
Ethical Practice Rules for Therapists: Applying Judgment in Complex Situations
Ethical practice is rarely tested in straightforward cases. It becomes relevant when there is no single correct decision, when client preferences, clinical judgment, and potential risk do not fully align.
In these situations, you are not applying a rule in isolation. You are weighing competing priorities, deciding how much to guide versus step back, and ensuring that your actions remain aligned with both client welfare and professional responsibility.
For experienced therapists, the challenge is not knowing ethical principles. It is applying them consistently when the situation is ambiguous.
Where ethical judgment becomes critical
Ethical decision-making tends to surface in specific types of situations where multiple factors overlap.
- When client choices conflict with your clinical view: You may believe a different course of action would be more beneficial, but the client’s autonomy still holds.
- When your personal values are activated: Certain topics or decisions may create internal reactions that can influence how you respond.
- When a case moves beyond your core competence: The difficulty is recognizing the limit early enough to act appropriately.
- When outcomes are uncertain: There is no clear right answer, only a defensible process.
Core ethical practice rules (and how to apply them in real work)
1. Respect client autonomy without withdrawing clinical responsibility: Supporting autonomy does not mean becoming passive. Your role is to help clients make informed decisions, not to make decisions for them. In practice, this means:
- clarifying options and potential consequences without directing outcomes
- checking whether the client fully understands implications
- continuing to engage even when you disagree with their choice
2. Do not impose personal beliefs or values: Ethical neutrality is not the absence of perspective. It is the ability to prevent your perspective from shaping the client’s decisions. In practice, this means:
- noticing internal reactions during sessions
- avoiding leading questions that steer toward your viewpoint
- separating clinical guidance from personal preference
3. Practice within your area of competence: Competence is not static. It shifts based on the client, context, and complexity of the issue. In practice, this means:
- recognizing early signs that a case exceeds your training
- seeking supervision or consultation when needed
- referring when the client’s needs cannot be met effectively within your scope
4. Remain objective and monitor bias continuously: Bias does not only affect diagnosis. It affects interpretation, response, and expectations. In practice, this means:
- questioning initial assumptions about the client’s situation
- reflecting on patterns in your responses across sessions
- using supervision to identify blind spots
5. Ensure decisions are consistent and defensible: Ethical decisions must hold up over time and under review. In practice, this means:
- documenting reasoning behind key decisions
- applying similar standards across similar cases
- avoiding reactive or inconsistent responses
What ethical practice looks like during sessions
Ethical work is not separate from clinical work. It is embedded in how you respond moment to moment.
- how you frame questions when exploring sensitive topics
- how much direction you provide when clients feel uncertain
- how you respond when a client’s decision creates potential risk
- how you balance empathy with maintaining clinical structure
These are micro-decisions, but they accumulate into the overall quality and integrity of care.
Where experienced therapists still encounter difficulty
Even with experience, certain patterns tend to appear:
- becoming overly directive when you feel confident about an outcome
- stepping back too much in the name of autonomy
- missing early signals that a case requires referral
- underestimating how personal bias influences subtle decisions
These are not errors in knowledge. They are gaps in ongoing reflection.
What strong ethical practice looks like
When ethical principles are applied well:
- clients retain ownership of their decisions
- your guidance remains clear but not controlling
- your responses are consistent across similar situations
- your decisions can be explained and justified if reviewed
If your process is structured, reflective, and consistent, your ethical practice is aligned.
Also Read:11 Group Therapy Techniques Every Therapist Should Use in 2026
Safety and Legal Rules for Therapists: How to Respond When Risk Is Involved
Safety-related decisions are where ethical practice becomes most time-sensitive. Unlike boundaries or general ethics, these situations often require action under uncertainty, with limited time to assess risk and consequences.
The difficulty is not knowing that safety comes first. It is determining when a situation has crossed the threshold that requires intervention, and what level of response is appropriate.
In these moments, your decisions need to balance immediacy, proportionality, and documentation.
Where safety and legal decisions become complex
These situations rarely present as clear-cut emergencies. More often, they develop gradually or appear ambiguous.
- When risk is present but not clearly imminent: You are deciding whether to monitor, intervene, or escalate.
- When client trust may be affected by action: Intervening may protect safety but impact the therapeutic relationship.
- When legal obligations vary by context: Your response may depend on jurisdiction, setting, or type of risk.
- When time is limited: You may need to act before full clarity is available.
Core safety and legal rules (and how to apply them in practice)
1. Prioritize safety when credible risk is identified: Safety takes precedence when risk reaches a level where inaction could result in harm. In practice, this means:
- assessing intent, plan, means, and immediacy
- not delaying action when risk is high
- initiating appropriate steps such as safety planning or escalation
2. Act based on risk thresholds, not uncertainty alone: Not all disclosures require intervention. The key is determining when risk becomes actionable. In practice, this means:
- distinguishing between ideation and imminent intent
- identifying protective factors and support systems
- using structured assessment rather than reacting to isolated statements
3. Limit action to what is necessary and proportionate: Interventions should match the level of risk, not exceed it. In practice, this means:
- choosing the least intrusive option that still ensures safety
- avoiding over-escalation when lower-level interventions are sufficient
- reassessing as the situation evolves
4. Document decisions and reasoning clearly: In high-risk situations, documentation is as important as the decision itself. In practice, this means:
- recording what was disclosed and how risk was assessed
- documenting why a specific action was taken or not taken
- maintaining a clear timeline of decisions and follow-ups
5. Stay aligned with legal and reporting obligations: Your response must reflect both ethical judgment and legal requirements. In practice, this means:
- being aware of mandatory reporting laws in your jurisdiction
- understanding duty-to-warn or duty-to-protect obligations
- ensuring actions are consistent with regulatory expectations
What strong safety practice looks like
In high-risk situations, clarity matters more than perfection. A strong approach allows you to:
- assess risk without overreacting or underreacting
- act decisively when thresholds are met
- explain and justify your decisions if reviewed
- maintain as much therapeutic trust as possible while prioritizing safety
Where experienced therapists still encounter difficulty
Even with experience, certain patterns tend to appear:
- hesitating when risk is ambiguous
- over-relying on client reassurance without full assessment
- under-documenting reasoning in urgent situations
- overcorrecting with overly aggressive interventions
These challenges are not about knowledge. They are about applying judgment under pressure.
Also Read: 18 Effective Person-Centered Therapy Techniques & Interventions
When Therapists Can Break Confidentiality: Decision-Making in Practice
Confidentiality is one of the strongest commitments you make in therapy, but it is not absolute. The difficulty is not identifying the exceptions. It is determining when a situation has crossed the threshold where maintaining confidentiality creates greater risk than breaking it.
In practice, these decisions rarely arrive as clear emergencies. More often, they emerge gradually. A client may disclose something concerning without clear intent, or a pattern may build across sessions that only becomes significant when viewed over time.
Your role is to interpret these signals, assess whether action is required, and respond in a way that is proportionate, legally sound, and clinically justified.
How to assess whether disclosure is required
Before acting, you are not simply reacting to what is said. You are evaluating whether the situation meets a threshold that requires intervention.
This typically involves weighing multiple factors together:
- Immediacy of risk: Is there a current likelihood of harm, or is the concern hypothetical or future-oriented?
- Level of intent and planning: Has the client moved from thoughts to preparation or capability?
- Presence of protective factors: Are there supports, relationships, or constraints that reduce risk?
- Specificity of the situation: Is there an identifiable person, timeframe, or method involved?
These factors are not assessed in isolation. A single statement rarely determines the outcome. It is the combination that informs whether confidentiality can be maintained or needs to be limited.
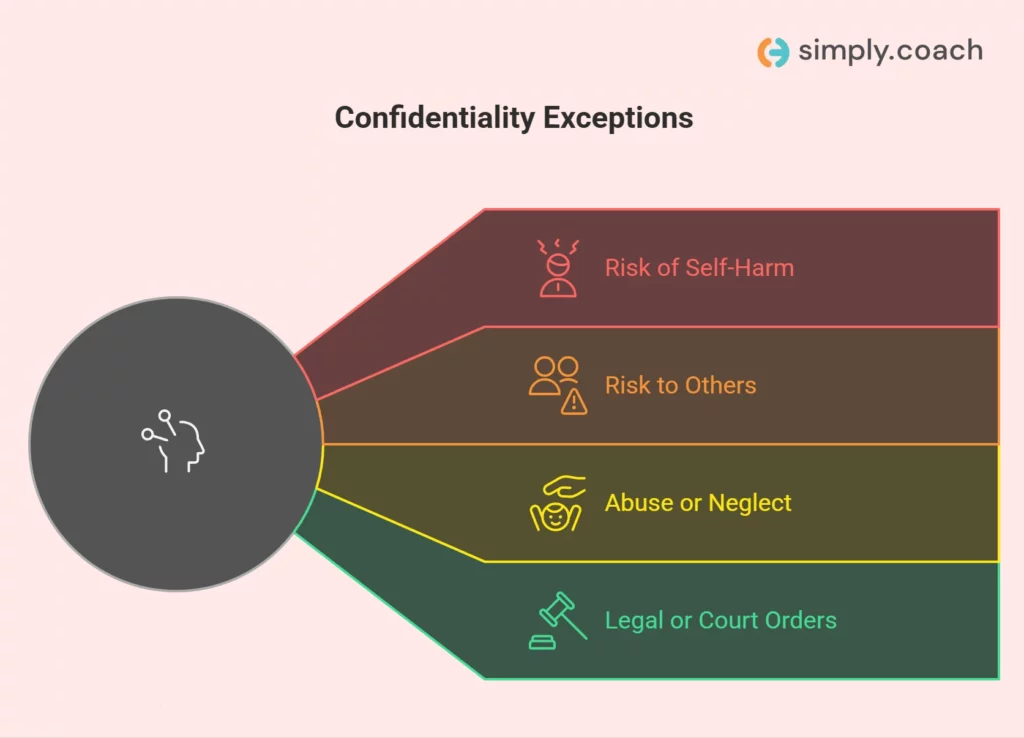
Situations where breaking confidentiality may be required
The categories are well-established, but the decision still depends on how you interpret the context in front of you.
1. Risk of harm to self: When a client expresses thoughts of self-harm, the decision is not whether risk exists. It is whether the risk is actionable.
If a client is expressing distress without intent or plan, your response may remain within the therapeutic space. As intent becomes clearer or protective factors weaken, your responsibility shifts toward intervention.
In practice, you are:
- assessing whether the client can maintain their own safety
- determining whether support systems are accessible
- deciding whether external intervention is necessary
The shift from ideation to imminent risk is often gradual, which is why ongoing assessment matters.
2. Risk of harm to others: Statements about harm toward others require careful interpretation. Not all expressions of anger or frustration indicate actionable risk.
The decision point is reached when there is a credible threat that is specific and preventable.
In practice, you are:
- evaluating whether a specific individual or group is identified
- assessing whether the client has the means and intent to act
- determining whether intervention can realistically prevent harm
This requires restraint as much as action. Overreacting can damage trust, while underreacting can create serious consequences.
3. Abuse or neglect (mandatory reporting): In cases involving vulnerable individuals, your responsibility is defined more clearly by law. However, the complexity often lies in recognition rather than action.
Clients may disclose indirectly, minimize experiences, or present incomplete information. You are required to interpret these signals and act when reasonable suspicion is present.
In practice, you are:
- identifying patterns that indicate possible harm
- understanding who qualifies under reporting requirements
- acting even when certainty is not absolute
Here, the threshold is not proof. It is a reasonable concern.
4. Legal orders and formal requests: When disclosure is required by law, your role shifts from interpretation to compliance, but not without boundaries.
You are still responsible for how information is shared and ensuring that disclosure remains limited to what is required.
In practice, you are:
- verifying the scope and validity of the request
- restricting disclosure to relevant information only
- informing the client when possible before action is taken
Even in legally mandated situations, discretion still applies.
5. Applying the minimum necessary disclosure principle: Breaking confidentiality does not mean sharing everything you know. One of the most important safeguards is limiting disclosure to what is required for the specific situation.
This requires active filtering of information.
- focus on facts relevant to the risk or legal requirement
- exclude unrelated clinical history or sensitive detail
- document exactly what was shared and why
This protects the client from unnecessary exposure and ensures your response remains proportionate.
Communicating the decision to the client
How you communicate a breach of confidentiality directly affects how the therapeutic relationship continues.
If the limits of confidentiality were clearly explained early on, the conversation becomes one of consistency rather than surprise. If not, the situation can feel abrupt or trust-breaking.
In practice, this means:
- explaining the reasoning in clear, direct terms
- referencing previously discussed limits of confidentiality
- avoiding framing the decision as optional when it is not
- remaining engaged with the client after the action
The goal is not to eliminate discomfort. It is to maintain transparency and clinical integrity.
Documentation: making your decision defensible
In situations involving disclosure, documentation becomes part of the ethical process, not just a record. Your notes should reflect how the decision was made, not just what was done.
This includes:
- what the client disclosed and in what context
- how risk was assessed across multiple factors
- why the threshold for action was met
- what action was taken and when
- who was informed and what was shared
Clear documentation ensures your decisions can be understood if reviewed later, especially in high-risk or legally sensitive cases.
Where experienced therapists still encounter difficulty
Even with experience, certain patterns tend to appear in these situations:
- waiting for certainty before acting when thresholds are already met
- reacting too quickly without structured assessment
- documenting actions without capturing reasoning
- not revisiting confidentiality limits after the initial consent process
These are not gaps in knowledge. They are gaps in how decisions are structured under pressure.
What strong practice looks like
When confidentiality limits are handled well, your decisions follow a clear internal logic. You can explain not just what you did, but why it was necessary and proportionate.
- actions are based on assessed thresholds, not assumptions
- disclosure is limited and intentional
- communication with the client is clear and consistent
- documentation reflects both decision and reasoning
If your process remains structured, even in high-pressure situations, your approach is aligned with both ethical and legal expectations.
Also Read:Top SimplePractice Alternatives for Therapists 2026
Common Boundary Violations in Therapy: Early Warning Signs to Watch For in 2026
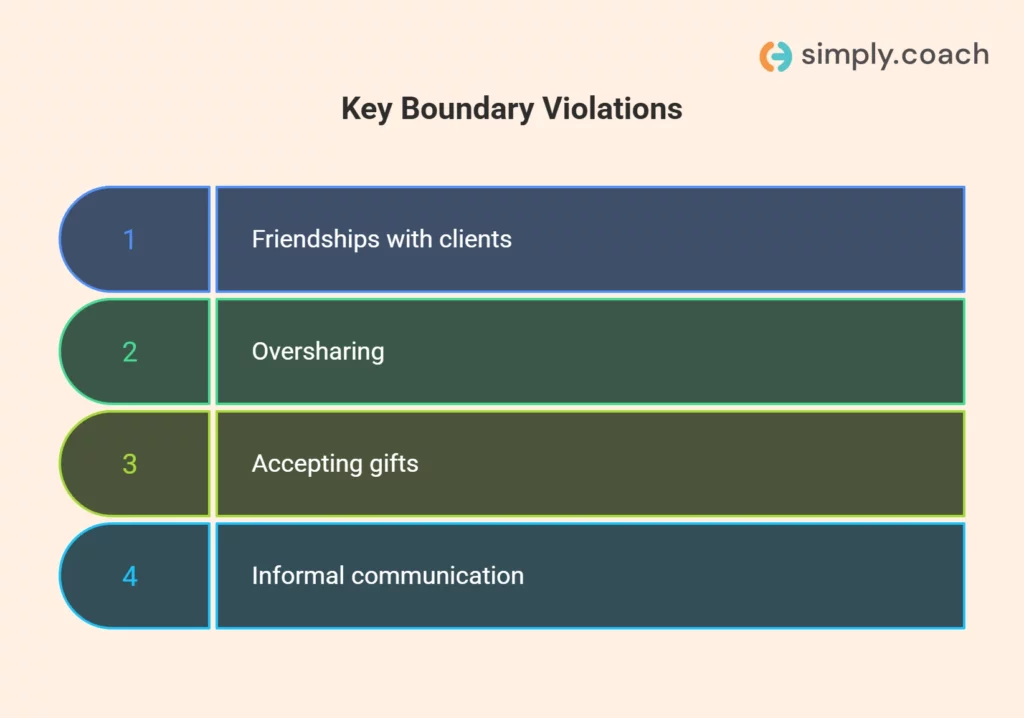
Boundary violations in therapy rarely begin as clear ethical breaches. They tend to emerge through small adjustments that feel reasonable in the moment but gradually shift the structure of the relationship. In long-term work, familiarity increases, communication becomes more fluid, and expectations expand without being explicitly reset.
The issue is not a single decision. It is the accumulation of these shifts that begins to affect objectivity, role clarity, and the therapeutic frame.
1. Unstructured communication outside sessions
One of the earliest signs of boundary drift is increased accessibility outside scheduled sessions. What begins as occasional check-ins can gradually turn into ongoing communication, especially in digital settings where messaging feels informal and immediate.
Over time, this changes expectations around availability and response, and clients may begin to rely on interaction outside the therapeutic space rather than within it.
In practice, this often looks like:
- responding to messages beyond agreed timeframes
- engaging in ongoing conversations instead of structured check-ins
- using multiple communication channels without clear boundaries
2. Shift toward informality in tone and interaction
As the therapeutic relationship develops, tone can become more relaxed. While rapport is important, a consistent shift toward informality can reduce the professional frame that supports the work.
This is not about avoiding warmth. It is about maintaining clarity in the relationship structure.
Early signals include:
- increased use of casual or personal language
- humor or interaction styles that move away from therapeutic intent
- sessions becoming less structured or goal-oriented
If not addressed, this can lead to role ambiguity and reduced clinical direction.
3. Self-disclosure without clear clinical intent
Self-disclosure can support therapy when used intentionally. The issue arises when it becomes frequent, reactive, or loosely connected to the client’s process.
In these cases, the focus begins to shift from the client’s experience to the therapist’s, often without clear benefit to the work.
In practice, this may involve:
- sharing personal experiences without a defined therapeutic purpose
- responding to client disclosures with parallel personal stories
- using disclosure to build connection rather than support outcomes
Over time, this can alter the power balance and reduce focus on the client.
4. Accepting gifts or gestures without evaluation
Gift-giving can carry meaning that goes beyond the gesture itself. Accepting gifts without exploring their context can introduce subtle expectations or obligations into the relationship.
This is particularly relevant in long-term work or culturally sensitive contexts.
Situations to pay attention to include:
- repeated or high-value gifts
- gifts given at moments of emotional intensity
- not discussing the meaning or intention behind the gesture
If left unexamined, this can influence neutrality and client expectations.
5. Gradual role shifts and over-involvement
Boundary drift often shows up as a shift in role rather than a clear violation. You may begin to take on functions beyond the therapeutic scope, especially when clients are struggling or dependent.
This shift is usually gradual and often justified in the moment.
Common patterns include:
- providing advice or direction outside therapeutic framing
- becoming overly invested in specific outcomes
- taking responsibility for decisions that belong to the client
Over time, this reduces client autonomy and increases emotional and professional strain.
How to respond when boundary drift appears
Boundary issues are easier to correct early than after they become established patterns. The response should be direct, proportionate, and grounded in the purpose of therapy.
In practice, this means:
- addressing the shift within the session as soon as it is noticed
- clarifying expectations around communication, roles, and structure
- linking boundaries to therapeutic effectiveness rather than authority
- documenting any boundary-related discussions or adjustments
What strong boundary practice looks like
Strong boundary management is not about rigidity. It is about maintaining a consistent structure that supports the work while adapting to context deliberately.
When boundaries are managed well:
- roles remain clear, even in long-term relationships
- communication stays predictable and contained
- clients understand the structure of engagement
- clinical decisions remain objective and consistent
If you are identifying shifts early and addressing them without delay, your boundary framework is functioning as it should.
Also Read:Self-Disclosure in Therapy – When and How Therapists Should Use It
Why Therapist Ethical Rules Matter More in 2026
The core ethical principles of therapy have not changed. Confidentiality, boundaries, and client welfare remain the foundation. What has changed is the context in which you are applying them.
In 2026, the same rules are being applied across more variable, less controlled environments. This increases the number of decisions you need to make, the speed at which you make them, and the level of accountability attached to them.
The shift is not theoretical. It shows up in how your day-to-day work is structured.
1. Therapy is no longer confined to a controlled setting
In traditional settings, you had more control over the therapeutic environment. Sessions happened in defined spaces, communication was contained, and confidentiality risks were easier to manage. That is no longer the case.
You are now working across:
- video platforms and remote environments
- messaging channels that extend beyond sessions
- client-controlled spaces where privacy cannot be fully ensured
This changes how you apply confidentiality and boundaries. You are not just managing what happens inside the session, but across every interaction point.
2. Data privacy is now part of clinical responsibility
Client awareness around data has increased significantly. Questions about where information is stored, who can access it, and how it is used are more common and more specific.
This shifts part of your role from passive compliance to active explanation.
In practice, this means:
- understanding how your tools store and process data
- being able to explain privacy practices clearly to clients
- ensuring documentation is both secure and appropriately limited
Ethical responsibility now includes how information is handled outside the session, not just what is discussed within it.
3. Boundaries extend beyond the therapy room
Boundaries are no longer limited to session time. Digital access, social platforms, and flexible communication have expanded the ways clients can interact with you.
This creates ongoing boundary decisions rather than fixed rules.
In practice, this shows up as:
- managing expectations around availability and response time
- maintaining separation between professional and personal digital presence
- deciding how and when communication outside sessions is appropriate
The challenge is not setting boundaries once. It is maintaining them consistently across different channels.
4. Practice contexts are more varied and overlapping
Many therapists now work across multiple formats, private practice, group work, digital programs, or cross-location clients. Each context can carry slightly different expectations and requirements.
This increases the complexity of applying ethical rules consistently.
You may find yourself:
- adapting consent and confidentiality based on format
- navigating different regulatory expectations across regions
- adjusting documentation practices depending on service type
The rule remains the same. The application changes with context.
5. Accountability and documentation standards are higher
Ethical decisions are no longer judged only by intent. They are evaluated based on how clearly they are documented and how consistently they are applied.
If a decision is questioned, what matters is not just what you did, but how you arrived at that decision. In practice, this requires:
- documenting reasoning, not just outcomes
- maintaining consistency across similar situations
- ensuring records are clear, structured, and retrievable
Good documentation is no longer optional. It is part of ethical practice.
What this means for your day-to-day work
The increase in complexity does not require new rules. It requires a more deliberate way of applying existing ones.
- you are making more decisions outside structured sessions
- you are managing more variables across tools and environments
- you are expected to explain and justify your approach more clearly
This shifts ethical practice from something you follow to something you actively manage.
What strong practice looks like in 2026
When ethical rules are applied well in modern practice:
- your decisions remain consistent across different contexts
- your boundaries hold even as communication channels expand
- your documentation reflects both action and reasoning
- your clients understand how their information is handled
If your approach remains structured, adaptable, and clearly documented, your practice is aligned with current expectations.
Also Read:WhySimply.Coach is the Best Life Coaching Platform for Your Business
How Simply.Coach Helps Therapists Stay Compliant and Maintain Ethical Practice
Ethical issues in therapy rarely come from not knowing the rules. They usually come from gaps in how information is recorded, accessed, and used across sessions.
If consent, session notes, communication, and client history are not structured, it becomes difficult to:
- apply confidentiality consistently
- document decisions clearly
- track what was disclosed and agreed
- maintain defensible records over time
Simply.Coach helps you structure your practice in a way that supports ethical consistency, especially in areas where documentation and communication matter most.
Where Simply.Coach directly supports ethical and compliant practice
- Client Workspaces (Session and Record Tracking): Every session, note, and client interaction is stored in one place. This allows you to review what was discussed, what decisions were made, and what context led to them, without relying on memory or scattered tools.
- Forms and Informed Consent Management: Consent forms, agreements, and client inputs are documented and accessible. This helps you clearly establish and revisit confidentiality limits, expectations, and permissions when situations require it.
- Session Notes and Clinical Documentation: Sessions are recorded with structure, allowing you to capture not just what happened, but why decisions were made. This is critical in situations involving risk, boundary adjustments, or disclosure.
- Secure Documentation and Data Handling: Client data is stored in a controlled environment, reducing the risk of exposure across multiple tools. This supports confidentiality not just during sessions, but across all data handling.
- Structured Communication and Scheduling: Client interactions are managed within defined channels, helping you maintain consistent boundaries around availability and communication outside sessions.
- Centralized Client History and Context: You can track patterns, past disclosures, and previous decisions over time. This supports consistency in how ethical rules are applied across sessions, rather than treating each interaction in isolation.
What this changes in practice
When your systems are structured:
- you can trace decisions back to context and documentation
- you maintain consistency in applying confidentiality and boundaries
- you reduce gaps caused by missing or fragmented information
- you can explain and justify your actions if reviewed
Simply.Coach does not replace ethical judgment. It ensures that the information behind your decisions is structured, accessible, and consistent.
Conclusion
Therapist ethical rules are not difficult to understand. The challenge is applying them consistently in situations that are not clearly defined.
In practice, most ethical decisions happen in small moments, how you interpret a disclosure, how you respond to a boundary shift, or how you document a situation that may later need explanation. Over time, these decisions shape how safe, consistent, and defensible your practice is.
Maintaining ethical consistency becomes easier when your practice is structured to support it.
Simply.Coach helps you keep client records, session notes, consent, and communication organized in one place, so your decisions are backed by clear, accessible documentation.
See how Simply.Coach supports ethical, structured therapy practice!
FAQs
1. How do therapists explain confidentiality limits to clients?
Therapists typically explain confidentiality and its limits during the informed consent process at the start of therapy. This includes outlining specific scenarios, such as risk of harm, abuse, or legal requirements, where disclosure may be necessary. Clear upfront communication helps set expectations and prevents misunderstandings later.
2. Are therapist rules different across countries or states?
Yes, while core ethical principles are broadly consistent, legal requirements vary by jurisdiction. For example, mandatory reporting laws, data privacy regulations, and licensing requirements can differ significantly. Therapists must stay informed about the rules specific to where they practice and where their clients are located.
3. How often should therapists review ethical guidelines?
Ethical guidelines should be reviewed regularly, especially when there are changes in regulations, technology, or scope of practice. Many experienced therapists revisit these standards during supervision, continuing education, or when encountering complex cases to ensure alignment with current best practices.
4. What should therapists do if they face an ethical dilemma?
In complex situations, therapists should refer to professional codes of ethics, seek supervision or peer consultation, and carefully document their reasoning. Taking a structured approach helps ensure that decisions are ethically sound, legally compliant, and defensible if questioned later.
5. Can therapists use messaging apps to communicate with clients?
Therapists can use messaging tools only if they meet required privacy and security standards. This includes ensuring encryption, secure storage, and clear boundaries around communication use. Informing clients about how these tools are used is also part of ethical practice.
6. How do therapists manage boundaries in long-term client relationships?
Over time, familiarity can blur professional lines, so therapists must actively maintain boundaries through clear communication and consistent behavior. Periodic reflection, supervision, and revisiting expectations with clients help preserve objectivity and the integrity of the therapeutic relationship.
7. What role does documentation play in ethical therapy practice?
Documentation is essential for continuity of care, risk management, and legal compliance. Detailed and accurate records support clinical decision-making and provide a clear account of actions taken, especially in complex or high-risk situations.
About Simply.Coach
Simply.Coach is an enterprise-grade coaching software designed to be used by individual coaches and coaching businesses. Trusted by ICF-accredited and EMCC-credentialed coaches worldwide, Simply.Coach is on a mission to elevate the experience and process of coaching with technology-led tools and solutions.
