As a therapist, the clinical work is a calling, but the billing process is a complex administrative hurdle. Managing insurance panels, navigating ‘Explanation of Benefits’ (EOB) documents, and ensuring compliance with payer rules requires as much precision as a treatment plan.
When the financial side of your practice feels strained, it is rarely due to a single major error. Instead, it is typically the result of small, compounding inefficiencies (denied claims that are not followed up, incorrect CPT codes like 90834 or 90837, or delays in reimbursements) that erode the practice’s bottom line and make cash flow unpredictable.
Whether you are navigating insurance panels, managing a private-pay model, or balancing a hybrid of both, billing functions as the primary operational system of your practice. It affects how quickly you get paid, the volume of your administrative burden, and your ability to track revenue across various clinical services.
In reality, most billing problems are not about complexity. They come from misalignment, using one workflow for different services, not updating systems as your practice evolves, or relying on tools without a clear structure behind them.
Updated for 2026, this guide breaks down billing for therapists with a focus on how it actually works in real practice. You will learn how to structure your billing across insurance, private pay, and hybrid models, use CPT codes accurately, and build a system that reduces errors while keeping payments consistent.
Key Takeaways
- Billing for therapists is a revenue system, not just an admin task, it directly impacts cash flow, compliance, and practice stability.
- The three core billing models are insurance, private pay, and hybrid, and the right choice depends on how your practice earns most of its revenue.
- Insurance billing requires accurate CPT codes (like 90834, 90837), ICD-10 diagnoses, and strong documentation to avoid denials.
- The “50% rule” helps simplify decisions; build your billing system around your primary revenue stream, then layer in others.
- Hybrid practices need separate billing workflows for therapy, coaching, programs, and consulting to maintain clarity and accuracy.
- Most billing issues come from misalignment; mixing services, using incorrect codes, or not updating systems as the practice evolves.
- A structured billing setup improves payment consistency, reduces errors, and gives clear visibility into which services drive growth.
- Simply.Coach
What Is Billing for Therapists and Why is it Relevant?
Billing for therapists is the process of charging clients or insurance providers for therapy services, whether through direct payments, insurance claims, or superbills. In practice, it is not just about sending a claim or invoice. It is the system that connects what you deliver in a session to how and when you get paid, while keeping your documentation, coding, and compliance aligned.
In day-to-day practice, billing is not a single step. It runs across your entire workflow, before the session, during documentation, and after submission or payment collection. Whether you are working with insurance or private pay, consistency across these steps is what determines how reliably you get paid.
For private-pay therapists, this includes invoicing, collecting payments upfront or post-session, and issuing superbills for out-of-network reimbursement. While payment is faster, the need for structured tracking and reconciliation remains.
Where billing actually shows up in your workflow
Billing is distributed across multiple operational points in your practice. Most issues arise when these are handled inconsistently or disconnected from each other.
- Insurance claims (CPT, ICD-10, and modifiers): Every claim depends on alignment between session time, diagnosis, and documentation. For example, using 90837 without clear time support or medical necessity often leads to denials or downcoding.
- Client invoicing and payment collection (private pay): This includes per-session billing, packages, and prepaid plans. The risk here is not denial, but gaps in tracking payments, refunds, or outstanding balances.
- Superbills for out-of-network clients: These require the same coding accuracy as insurance claims. Errors shift the burden to the client and can impact their reimbursement.
- Payment tracking, copays, and deductibles: Especially with insurance, what is billed is not what you receive. You need to track insurer payments, client responsibility, and adjustments to avoid revenue leakage.
- Revenue reconciliation and reporting: Matching billed vs received amounts is where inconsistencies surface. This is critical in hybrid practices where multiple billing flows exist.
At the same time, it is important to understand what billing does not do. Billing systems execute your inputs, but they do not validate whether your inputs are correct or complete.
Errors in eligibility, coding, or documentation often surface only after submission, when claims are denied, delayed, or partially paid.
What billing does not do (and where mistakes happen)
- It does not ensure reimbursement without documentation alignment: Even correctly submitted claims can be denied if your notes do not support session duration, diagnosis, or medical necessity.
- It does not replace clinical or compliance requirements: Billing depends on your clinical records. If documentation is inconsistent, billing accuracy breaks down.
- It does not fix pricing, positioning, or revenue gaps: If your service mix or pricing model is misaligned, billing will reflect those issues, not solve them.
Here is the reality for most therapists: billing is rarely one-dimensional. Many practices operate across insurance, private pay, and additional services like programs or workshops. Each of these follows a different billing logic, claims-based, invoice-based, or product-style payments.
When these are forced into a single workflow, visibility drops. You may still get paid, but you lose clarity on where delays, denials, or inconsistencies are coming from.
The more reliable approach is to structure your billing around your primary revenue source. If most of your income comes from insurance, your system should prioritize claims, coding accuracy, and denial tracking. If it comes from direct payments, invoicing and collection should be the foundation.
This alignment is what reduces errors, improves payment consistency, and gives you a clear view of how your practice is actually generating revenue.
Also read: How to Understand the 8 Minute Rule for Medicare Billing in Therapy
3 Main Types of Billing for Therapists
When it comes to billing for therapists, most practices operate within three models: insurance-based billing, private pay, and hybrid. The models themselves are straightforward. The challenge is choosing the one that aligns with how your practice actually earns and collects revenue.
The mistake is treating this as a preference decision. In practice, your billing model should follow your revenue pattern, not the other way around. Each model behaves differently in terms of payment timing, administrative load, and risk of errors.
1. Insurance-based billing (high volume, delayed payment, higher admin)
Insurance billing is structured around claims. You submit services using CPT codes like 90834 or 90837, supported by ICD-10 diagnoses and clinical documentation. Payment is processed later, often with adjustments, denials, or partial reimbursements.
This model works when your practice is designed around consistency and volume. It requires tight alignment between documentation, coding, and submission workflows.
In practice, this model involves:
- Verifying eligibility, copays, and authorizations before sessions
- Documenting medical necessity clearly in clinical notes
- Selecting CPT codes based on actual session duration
- Submitting claims and tracking denials or resubmissions
Where it works well:
- You are credentialed with insurance panels
- Your client base depends on coverage and affordability
- You are set up to handle ongoing claims and follow-ups
Where it breaks:
- Documentation does not support billed services
- Claims are submitted but not tracked
- Denial patterns are not reviewed or corrected
The tradeoff is clear: predictable client volume vs delayed and administratively heavy revenue.
2. Private pay billing (low friction, immediate payment, pricing control)
Private pay removes the claims layer. Clients pay directly for sessions, either per session, in packages, or through prepaid plans. You may still provide superbills, but reimbursement responsibility shifts to the client.
This model simplifies billing, but it shifts responsibility toward pricing clarity and payment discipline.
In practice, this model involves:
- Setting clear session rates or package pricing
- Collecting payment upfront or immediately post-session
- Issuing invoices, receipts, or superbills when needed
- Tracking payments and outstanding balances consistently
Where it works well:
- You want faster, predictable cash flow
- Your services extend beyond insurance-covered therapy
- You prefer operational simplicity over administrative load
Where it breaks:
- Payments are not collected consistently
- Pricing is unclear or varies across clients
- Revenue tracking is not structured across sessions or packages
The tradeoff: speed and control vs reduced accessibility for some clients.
3. Hybrid billing model (flexibility with added complexity)
Hybrid practices combine insurance and private pay. You may accept insurance for core therapy while offering private-pay services such as programs, intensives, or out-of-network sessions.
This is the most common model as practices grow, but it introduces complexity because you are managing two billing systems at once.
In practice, this model involves:
- Running parallel workflows for claims and invoicing
- Separating clinical services from non-covered services
- Tracking revenue across different payment timelines
- Managing both insurer payments and direct client payments
Where it works well:
- Your services span clinical and non-clinical offerings
- You want both accessibility (insurance) and flexibility (private pay)
- You have systems to track multiple revenue streams clearly
Where it breaks:
- Insurance and private-pay workflows are mixed together
- Services are billed incorrectly under the wrong model
- Revenue tracking does not distinguish between sources
The tradeoff: maximum flexibility vs higher operational complexity.
What matters more than the model itself
The model does not determine success. Alignment does.
- Your billing workflow should match how money flows into your practice
- Your documentation should support how services are billed
- Your tracking should reflect when and how payments are received
When these are aligned, billing becomes predictable. When they are not, issues show up as denials, delays, or unclear revenue patterns.
Also Read: 10 Best Therapist Billing Software In 2026
Billing for Therapists with Multiple Services: Setup and Use Cases
As therapy practices evolve, billing for therapists becomes less about choosing a single method and more about structuring billing across different services. Most top-ranking content focuses heavily on insurance workflows, but in reality, many therapists today operate hybrid practices, combining therapy, coaching, programs, consulting, or partnerships.
The challenge begins when everything is forced into one billing model. That may work in the early stages, but as services expand, it creates friction; unclear revenue tracking, billing inconsistencies, denied claims, and gaps in payments. Over time, this is not just an operational issue; it becomes a visibility problem, where you can no longer clearly see how your practice is actually generating income.
A simple rule helps bring clarity:
Pick the billing model that matches what clients mostly pay you for.
Think of it as a 50% test. If most of your revenue comes from insurance, your system should be built around claims, coding, and reimbursement tracking. If most comes from direct client payments, invoicing and upfront payments should be the foundation.
If your revenue is split, a hybrid approach works, but it still needs a clear anchor. This prevents overcomplication while keeping your system aligned with how money flows.
1. Therapist–coach hybrid practice
This is one of the most common modern setups, where therapists combine clinical work with coaching or non-clinical services. On the surface, it may seem manageable under one system, but these services operate under fundamentally different billing rules.
Clinical therapy requires structured documentation, CPT codes, and diagnosis-based justification. Coaching does not. When these are blended into the same workflow, it creates confusion, both in how services are delivered and how they are billed.
A more stable approach is to separate the two clearly. Therapy should follow insurance or session-based billing with proper documentation, while coaching should follow private-pay models such as invoicing or packaged pricing. The overall billing structure should then reflect whichever side contributes the majority of your revenue.
It is also important to note that billing clinical services without appropriate licensure introduces compliance risks and increases the likelihood of claim denials.
2. Therapist + HR or organizational consulting
As therapists move into organizational work, such as workplace wellbeing programs or advisory, billing shifts away from session-based logic into contract-based structures. This is not just a change in how you bill, but in how revenue is recognized and managed.
Unlike therapy sessions, this work is often tied to deliverables, timelines, or retainers. Payments may be milestone-based or recurring, and there is no direct link to CPT codes or clinical documentation.
Trying to fit this into a session-based billing system leads to fragmentation. A clearer approach is to treat organizational work as a separate billing lane, using contracts and invoicing. If this type of work becomes a significant portion of your revenue, your billing system should gradually shift to reflect that, moving away from session-centric structures.
3. Therapist + course creator or program-based services
Programs and digital offerings introduce another layer of complexity because they sit between services and products. Many therapists struggle here because the billing model depends heavily on how the program is delivered.
Live or cohort-based programs often resemble session-based delivery, where payments may be tied to timelines or installments. In contrast, self-paced courses behave more like products, with upfront payments and no direct link to therapist time.
When these are treated the same as therapy sessions, revenue tracking becomes distorted. A more effective structure is to separate program revenue from clinical income and align billing with delivery. This creates clarity not only in accounting but also in understanding which parts of your practice are scalable and profitable.
4. Therapist + speaking or workshops
When workshops or speaking engagements become a consistent part of your practice, billing shifts from session-based to event-based. Revenue is no longer tied to individual client interactions but to engagements, contracts, and deliverables.
This requires a different mindset. Instead of billing per session, you are working with flat fees, deposits, and staged payments. There is no role for clinical codes or insurance processes here, and trying to apply them creates unnecessary complexity.
Separating event-based billing from therapy billing ensures that both remain clean and manageable, while also giving you clearer visibility into how this revenue stream contributes to your overall practice.
5. Therapist + referral, placement, or partnership income
In some practices, revenue comes from referrals, partnerships, or placement-style arrangements. This type of income is often irregular and does not follow the predictable patterns of sessions or programs.
The main challenge here is lack of structure. Without clear billing and tracking, this income can easily get mixed with core therapy revenue, making it difficult to understand its impact or maintain consistency.
A more structured approach is to treat this as a separate category altogether, using invoicing, agreements, and clear documentation. If it becomes a meaningful part of your income, your billing system should evolve to accommodate it rather than forcing it into existing workflows.
The underlying principle across all of these scenarios is clarity. Billing systems do not need to be complex, but they do need to reflect how each service is delivered and paid for. When that alignment is in place, errors reduce, tracking improves, and revenue becomes more predictable.
In one line: Anchor your billing system to your primary revenue source, then layer in secondary services without forcing them into the same structure.
Also Read: Best Mental Health Software for 2026: Top Platforms Compared
How to Choose the Right Billing Model for Your Therapy Practice
Choosing the right system for billing for therapists is not about picking between insurance or private pay in isolation, it is about aligning your billing with how your practice actually generates, documents, and collects revenue.
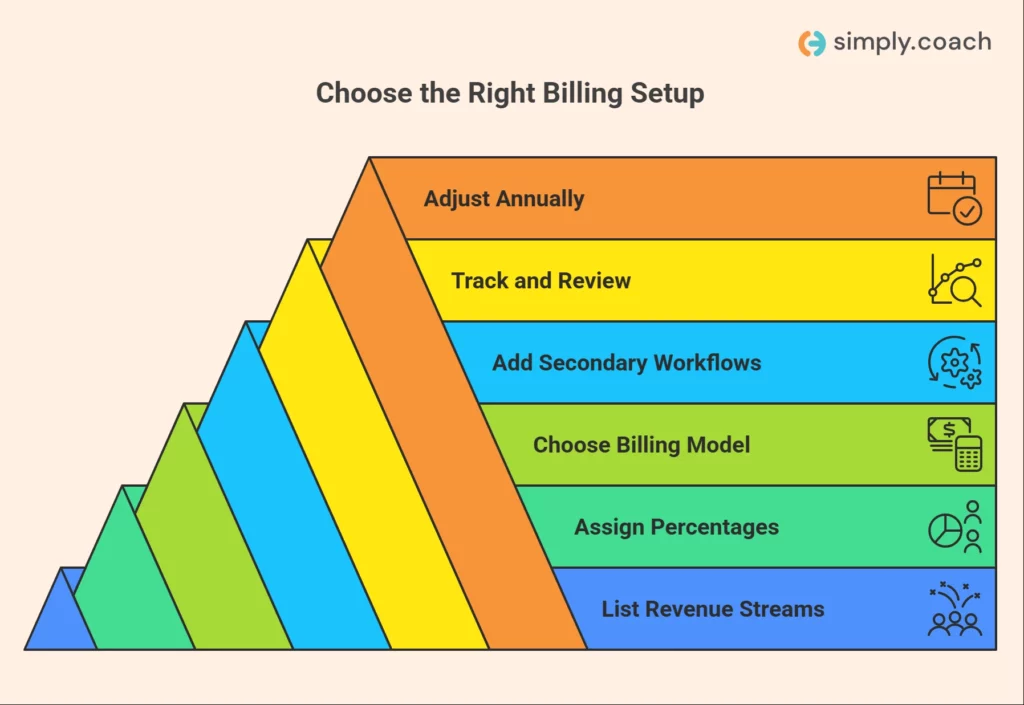
Most billing problems like denials, delayed payments, inconsistent tracking happen when there is a mismatch between your revenue model and your billing structure. This framework helps you remove that mismatch and build a system that is both accurate and scalable.
Step 1: List your revenue streams from the past year
Start by mapping out every way your practice earned money over the last 6–12 months. Go beyond just “sessions” and break it down by type.
Include:
- Insurance-based therapy (claims submitted with CPT codes like 90834, 90837)
- Private-pay sessions (direct client payments)
- Out-of-network clients (superbills issued)
- Group therapy or workshops
- Coaching or non-clinical services
- Online programs or courses
Why this matters: Each of these streams follows a different billing logic; claims, invoices, or product-style payments. If you treat them the same, your tracking and reporting will be inaccurate.
Step 2: Assign a percentage to each revenue stream
Estimate how much each stream contributes to your total income.
Example:
- 60% insurance billing
- 25% private pay
- 10% group programs
- 5% other
You do not need exact accounting-level precision. The goal is to identify your dominant revenue driver.
What to look for:
- Is most of your income delayed (insurance reimbursements)?
- Is it immediate (client payments)?
- Is it mixed across multiple formats?
This determines how your billing system should be structured.
Step 3: Choose the billing model that fits the largest share
Now align your billing setup with the revenue stream that contributes the most.
- Insurance-dominant practices: Build around claims workflows; eligibility verification, CPT/ICD-10 coding, documentation, claim submission, and denial tracking
- Private-pay dominant practices: Focus on invoicing, payment collection, packages, and simple revenue tracking
- Mixed (hybrid) practices: Use both, but anchor your system around the primary source and layer in the secondary
Key insight: Your primary billing model should reduce friction for your main revenue stream; not try to equally optimize everything.
Step 4: Add structured workflows for secondary revenue
If 20–40% of your income comes from a different type of service, you need to support it without disrupting your core system.
Examples:
- Insurance + private pay → separate claim workflows from invoicing workflows
- Therapy + programs → track program revenue independently from session billing
- Therapy + consulting → introduce contract-based invoicing alongside session billing
What this prevents:
- Mixing clinical and non-clinical services under the same billing logic
- Incorrect coding or documentation
- Loss of visibility into which services are actually driving revenue
The goal is clear separation, not complexity.
Step 5: Build in tracking and review checkpoints
Billing is not just about sending claims or invoices, it is about monitoring performance.
Set a monthly or quarterly review:
- Are claims being paid on time?
- Are there recurring denials (e.g., incorrect CPT codes, missing documentation)?
- Are payments aligned with what was billed?
- Which services are generating the most consistent revenue?
This turns billing into a feedback system, not just an admin task.
Step 6: Revisit and adjust annually
Therapy practices evolve; new services, new client types, new revenue streams. Your billing system needs to evolve with it.
Review once a year:
- Has your revenue mix shifted (e.g., more private pay, less insurance)?
- Have you added programs, courses, or B2B work?
- Is your current system still giving you a clear financial picture?
If not, adjust your structure, not just your tools.
The goal is to build a billing system that reflects how your practice actually operates. When your billing aligns with your revenue, everything becomes easier: fewer errors, faster payments, and clearer financial visibility.
Structure your billing around your primary revenue stream, support secondary services with clear workflows, and revisit the system as your practice grows.
Also Read: 11 Group Therapy Techniques Every Therapist Should Use in 2026
Why Billing Setup Matters for Therapists: Impact on Revenue in 2026
Your billing system is not just an administrative layer, it directly affects how your practice gets paid, how smoothly it operates, and how it is evaluated by external stakeholders. From insurance reimbursements to financial reviews and compliance checks, billing sits at the center of your revenue flow.
When your billing setup is aligned with how your services are delivered and paid for, it reduces friction across the board. When it is not, small inconsistencies can turn into denied claims, delayed payments, or operational slowdowns.
1. Insurance reimbursements, claims, and revenue stability
When it comes to billing for therapists, your setup directly affects how consistently you get paid. Insurance providers rely on structured billing like CPT codes, ICD-10 diagnoses, documentation, and eligibility verification to assess claims and determine reimbursement.
Why insurers care:
- Billing helps validate medical necessity
- Codes determine what services are eligible for reimbursement
- Documentation supports claim approval
What goes wrong with the wrong setup:
- Claims get denied due to incorrect or mismatched codes
- Payments are delayed because of missing documentation
- Reimbursements fall into the wrong category or rate
- Repeated errors can lead to audits or stricter reviews
Even small inconsistencies like incorrect session duration codes (e.g., 90834 vs 90837) can impact how and whether you get paid.
2. Loans, grants, and financial visibility
Your billing system also affects how your practice is evaluated financially. Whether you are applying for a loan, seeking funding, or simply working with an accountant, your revenue records need to be clear and consistent.
How billing impacts this:
- Clean billing records show predictable income patterns
- Lenders and institutions assess revenue stability based on your reports
- Organized financial data supports applications and approvals
If your billing is inconsistent or unclear, it becomes harder to demonstrate:
- How much you actually earn
- How stable your income is
- Whether your practice is financially sustainable
3. Banking, payment processors, and operational friction
Banks and payment processors may not evaluate your billing method directly, but they do monitor transaction patterns and reported income.
Where issues can arise:
- Reported income does not match actual deposits
- Irregular payment patterns raise internal checks
- Inconsistent records create delays in approvals or reviews
Misalignment does not always lead to rejection, but it can create review flags that slow down processes like account approvals, payment processing, or financial verification.
4. Compliance, documentation, and audit readiness
Billing is closely tied to compliance, especially for therapists working with insurance.
Why this matters:
- Claims must be backed by accurate clinical documentation
- Session details (time, intervention, notes) must align with billing codes
- Inconsistencies can trigger audits or claim disputes
A structured billing system ensures that:
- Your documentation supports your claims
- Your records are consistent over time
- You are prepared if your practice is reviewed
5. Business decisions and growth clarity
Beyond compliance and payments, billing plays a key role in how you understand and grow your practice.
With the right setup, you can:
- See which services generate the most revenue
- Identify delays or gaps in payments
- Adjust pricing based on actual data
- Plan expansion (programs, team, services) with confidence
Without that clarity, it becomes difficult to make informed decisions; everything starts to rely on assumptions rather than data.
6. Scaling without revenue confusion
As your practice grows, billing complexity increases; more clients, more services, and potentially multiple revenue streams.
If your billing system is not structured properly:
- Tracking becomes fragmented
- Revenue sources get mixed
- Financial reporting becomes unreliable
A well-aligned billing setup allows you to scale without losing visibility or control.
Your billing setup does more than process payments; it determines how reliably you get paid, how clearly you track revenue, and how confidently you can grow your practice.
Also Read: 18 Effective Person-Centered Therapy Techniques & Interventions
Top Billing Mistakes Therapists Make, and How to Avoid Them
At a more advanced level, issues in billing for therapists are rarely about missing steps; they come from structural gaps in how billing is set up and managed over time.
As your practice grows across insurance, private pay, and programs, these gaps start to affect revenue predictability, compliance, and decision-making.
Below are the most common patterns, and how to correct them with a more deliberate approach:
1. Treating all services under one billing system
One of the most common mistakes is applying a single billing logic across therapy, coaching, programs, and consulting. While this may feel efficient, it creates confusion in both tracking and reporting.
Each service type operates differently. Insurance billing depends on claims, documentation, and reimbursement cycles. Private pay is immediate and transaction-based. Programs and courses often follow cohort or product-style revenue.
When these are merged into one system, you lose clarity on what is actually driving revenue and where issues are occurring.
The fix is to create separate billing workflows for each service category, even if they run within the same tool. This allows you to track performance, reduce errors, and maintain consistency as your practice scales.
2. Using clinical codes without full documentation alignment
CPT and ICD-10 codes are not just administrative requirements, they represent a contract between your documentation and what you are billing.
A common issue is subtle misalignment:
- Session duration does not fully support the selected CPT code
- Clinical notes do not clearly justify medical necessity
- Interventions are not well linked to diagnosis
These issues may not show up immediately but often surface as denials or audits.
A stronger approach is to treat coding as a documentation-backed system. Your notes, time tracking, and billing codes should consistently reinforce each other. This reduces risk and improves claim acceptance rates over time.
3. Not updating billing as the practice evolves
Billing systems are often set up early and left unchanged, even as the practice expands into new services. Over time, this creates a mismatch between how revenue is generated and how it is tracked.
For example, adding programs, workshops, or B2B services without adjusting billing workflows leads to mixed revenue categories and unclear reporting.
The solution is to treat billing as something that evolves with your business model. Any meaningful shift in revenue like new services, different payment timing, or changes in client mix should trigger a review of your billing structure.
4. Over-reliance on tools without owning the system
Many therapists rely heavily on EHRs or billing platforms, assuming the system will handle complexity by default. While tools are essential, they do not define your billing logic, they only execute it.
This becomes a problem when:
- Default configurations do not match your service mix
- Errors go unnoticed because workflows are not clearly defined
- Teams follow the tool instead of a standardized process
The better approach is to define your billing logic independently, like how codes are selected, how services are categorized, and how workflows operate, then configure your tools to support that structure.
5. Not separating and tracking revenue by service line
As practices grow, total revenue becomes less useful than where that revenue is coming from. Without separation, it becomes difficult to assess which services are sustainable, profitable, or worth scaling.
For instance, insurance may drive volume but involve delays and lower margins, while programs may generate higher-margin revenue with different delivery effort.
Without clear separation, these dynamics remain hidden.
The fix is to track revenue at a more granular level by service type, payment model, and delivery format. This creates visibility that supports better pricing, positioning, and growth decisions.
6. Not documenting billing logic for consistency
In many practices, billing decisions exist as habits rather than documented systems. This works in the short term but creates inconsistency over time—especially when you introduce support staff or scale operations.
Without documentation:
- Code selection may vary between sessions
- Revenue categorization becomes inconsistent
- Audits or reviews become harder to manage
Creating a simple internal billing playbook covering workflows, coding logic, and categorization rules ensures consistency and makes your system easier to maintain and scale.
7. Treating billing as admin instead of a revenue system
Perhaps the most important shift is how billing is viewed. When treated as a background task, issues like denials, delays, and underpayments often go unnoticed.
At scale, billing should function as a performance system, one that provides visibility into:
- Payment timelines
- Claim acceptance patterns
- Revenue consistency
This allows you to identify inefficiencies early and optimize how your practice gets paid.
When billing is structured intentionally, aligned to your services, documented clearly, and reviewed regularly, it becomes a source of clarity rather than friction.
Strong billing systems are not just accurate, they are structured, visible, and aligned with how your practice actually generates revenue.
How Simply.Coach Supports Accurate Billing and Revenue Tracking
Billing issues in therapy rarely come from one step. They usually come from gaps across the workflow, sessions delivered but not tracked properly, documentation that does not align with billing, or payments that are not reconciled against what was billed.
As your practice grows across insurance, private pay, and programs, these gaps increase. Without a structured system, it becomes harder to:
- track what was delivered vs what should be billed
- maintain consistency between session notes and billing inputs
- manage multiple payment models without mixing workflows
- reconcile payments across claims, invoices, and programs
Simply.Coach helps you structure the operational side of your practice so your billing stays aligned with what you deliver.
Here’s how Simply.Coach supports billing consistency and revenue tracking:
- Client workspaces (session-to-billing alignment): Every session, note, and client interaction is stored in one place. This makes it easier to track what was delivered and ensure it matches what you bill, especially when working across multiple clients and services.
- Session notes and documentation (support for accurate billing): Structured notes help you maintain consistency in session duration, interventions, and client progress. This reduces mismatches between documentation and billing inputs, which are a common cause of claim denials.
- Programs and journeys (separate billing for structured services): For programs, packages, or cohort-based services, you can manage delivery separately from 1:1 sessions. This helps you avoid mixing program revenue with session-based billing and improves clarity in tracking.
- Scheduling and session tracking (reduce missed or unbilled sessions): Sessions are tracked systematically, making it easier to identify completed, upcoming, and missed sessions. This reduces revenue leakage from sessions that are delivered but not billed.
- Centralized client history (consistency across billing decisions): You can review past sessions, notes, and engagement patterns in one place. This supports consistent billing decisions, especially in hybrid practices where services differ across clients.
What this changes in your billing workflow
When your practice is structured:
- you can match sessions delivered with billing more reliably
- documentation stays aligned with what you charge
- different services follow separate, clear billing logic
- revenue tracking becomes consistent across payment models
Simply.Coach does not handle billing directly. It ensures that the inputs into your billing system, sessions, documentation, and client data, are structured, consistent, and reliable.
Conclusion
Billing for therapists becomes manageable when your system reflects how your practice actually delivers and gets paid for services.
Most issues do not come from complexity. They come from misalignment, sessions that are not tracked properly, documentation that does not support billing, or multiple services being forced into the same workflow. Over time, these gaps show up as denied claims, delayed payments, or unclear revenue patterns.
Billing works best when your practice operations are structured to support it.
Simply.Coach helps you organize sessions, documentation, and client activity in one place, so your billing stays aligned with what you deliver, without relying on scattered tools or manual tracking.
FAQs
1. What is the difference between CPT codes 90834 and 90837?
The difference is based on session length. 90834 is typically used for 45–55 minute sessions, while 90837 applies to sessions lasting 56 minutes or longer. Accurate time documentation is essential, as mismatches between notes and codes can lead to claim denials.
2. What information is required to bill insurance for therapy?
To submit a claim, therapists typically need the client’s insurance details, CPT code, ICD-10 diagnosis, session notes, and their NPI number. Proper documentation must support medical necessity and align with the billed service.
3. How do therapists verify insurance benefits before a session?
Therapists verify benefits by contacting the insurance provider or using billing software to check coverage, copays, deductibles, and authorization requirements. This step helps avoid unexpected costs for clients and reduces claim rejections.
4. What is a superbill and when should therapists use it?
A superbill is a detailed receipt that includes CPT codes, diagnosis, and provider information. It is used by out-of-network therapists so clients can submit it to their insurance for reimbursement.
5. Why do therapy insurance claims get denied?
Common reasons include incorrect CPT or ICD-10 codes, missing documentation, lack of medical necessity, or eligibility issues. Denials often point to mismatches between what was billed and what was documented.
6. Do therapists need billing software to manage claims?
Billing software is not mandatory, but it simplifies workflows such as claim submission, tracking reimbursements, and managing documentation. As practices grow, software becomes more useful for reducing manual errors and saving time.
7. Can therapists bill insurance for telehealth sessions?
Yes, telehealth sessions can be billed using standard CPT codes along with specific modifiers (such as modifier 95). Requirements vary by payer, so it is important to verify coverage and documentation standards beforehand.
About Simply.Coach
Simply.Coach is an enterprise-grade coaching software designed to be used by individual coaches and coaching businesses. Trusted by ICF-accredited and EMCC-credentialed coaches worldwide, Simply.Coach is on a mission to elevate the experience and process of coaching with technology-led tools and solutions.
