Starting a group therapy practice can feel like stepping into uncharted territory, even for seasoned clinicians. You might be wondering how to manage multiple clients, keep sessions structured, and maintain clinical safety, all without losing the depth and impact of your work. Balancing therapy, logistics, and client dynamics can quickly become overwhelming if not approached strategically.
If you’ve been thinking about expanding beyond one-on-one sessions, you know that group therapy comes with its own challenges: making sure everyone participates, handling emotional escalations, and applying interventions that actually work in a multi-client setting. Getting this right requires thoughtful planning, real-world judgment, and frameworks that you can trust to guide your decisions.
In this article, we’ll walk you through exactly how to start a group therapy practice, share practical decision-making frameworks, and learn actionable steps to structure group sessions.
Key Takeaways
- Structuring your group therapy practice with defined populations and modalities ensures high clinical fidelity and effective therapeutic outcomes.
- Evidence-based frameworks like DBT, ACT, and mindful self-compassion improve cohesion, interpersonal learning, and symptom reduction across group participants.
- Operational systems, SOPs, scheduling, action tracking, and co-facilitator coordination are essential to reduce no-shows and maintain consistent therapeutic quality.
- Screening, participant selection, and ongoing monitoring mitigate clinical risks, prevent destabilizing dynamics, and maintain group cohesion.
- Platforms like Simply.Coach integrates client management, goal tracking, action plans, scheduling, and reporting, allowing you to scale multiple groups without compromising care.
What Is A Group Therapy Practice?
A group therapy practice is a model in which you work with multiple clients in a structured setting, rather than running only one-on-one sessions. Each session is guided by you, but clients also learn from each other through shared experiences and discussions.
For you as a therapist, this shifts your work from purely individual sessions to a more leveraged format. You can support multiple clients simultaneously while maintaining a high level of engagement and accountability.
This model is best suited for clients who benefit from shared perspectives, structured guidance, and consistent support, especially in areas like relationships, behavior change, and emotional regulation.
Also read: How to Write Group Therapy Notes: Examples, Templates & Best Practices
8 Benefits of Starting a Group Therapy Practice
Launching a group therapy practice allows you to multiply your clinical impact while observing interpersonal dynamics in real time. If you’re an experienced therapist, you can integrate specialized interventions, facilitate peer modeling, and track collective behavioral change.

- Enhanced relational insights – You can observe transference, attachment patterns, and relational dynamics among clients, enabling interventions that would be limited in one-on-one sessions.
- Vicarious learning opportunities – Clients gain insight by witnessing peers overcome challenges, which encourages normalization, hope, and adaptive coping.
- Scalable clinical impact – Groups allow you to deliver interventions to multiple clients simultaneously without compromising treatment fidelity.
- Integration of advanced modalities – Incorporate DBT, ACT, psychodrama, IPT, or mindful self-compassion interventions cohesively across participants, enhancing clinical versatility.
- Skill generalization and reinforcement – Group settings provide repeated, real-time opportunities to practice emotion regulation, interpersonal skills, and behavioral strategies under guided supervision.
- Structured session frameworks – Stage-based progression (orientation, working, catharsis, problem-solving, termination) creates predictability while supporting dynamic clinical processing.
- Peer support and accountability – Clients reinforce each other’s growth, reducing isolation and improving adherence to therapeutic goals between sessions.
- Professional growth for therapists – Running groups hone facilitation, observational, and feedback skills, expanding your clinical repertoire and confidence with complex interventions.
Knowing the benefits provides the foundation for designing each session stage to ensure consistency and meaningful client progress.
Also read: 11 Group Therapy Techniques Every Therapist Should Use in 2026
Questions to Help You Decide Whether to Start a Group Practice
Starting a group therapy practice requires careful consideration of clinical, operational, and financial factors. Asking the right questions helps you anticipate challenges, structure your practice effectively, and ensure high-quality client outcomes.
- Do you have the clinical confidence to manage group dynamics? You should be comfortable handling multiple clients, emotional intensity, and peer interactions within the same session.
- Do you have basic systems in place? Scheduling, payments, communication, and session tracking should be organised enough to handle multiple clients without confusion.
- Is there a clear demand for your group’s offer? You should have a defined audience and problem area where clients are willing to join a shared format.
- Do you know how your group will make money? Your pricing, capacity per group, and expected revenue should be clear before you launch.
- Can you consistently fill and manage groups? Running groups requires steady client flow and the ability to maintain engagement over time.
- Are you ready to start simple and refine? You do not need a perfect setup. Starting with one group and improving based on real feedback is often the most effective approach.
If you can answer most of these clearly, you are in a strong position to start and build your group practice gradually.
7 Steps To Start a Successful Group Therapy Practice
Creating a group therapy practice requires integrating advanced clinical frameworks with precise operational planning. Each decision, from group composition to session design, affects therapeutic outcomes and safety. Proper structuring allows you to provide high-quality, evidence-based interventions while maintaining practice sustainability.
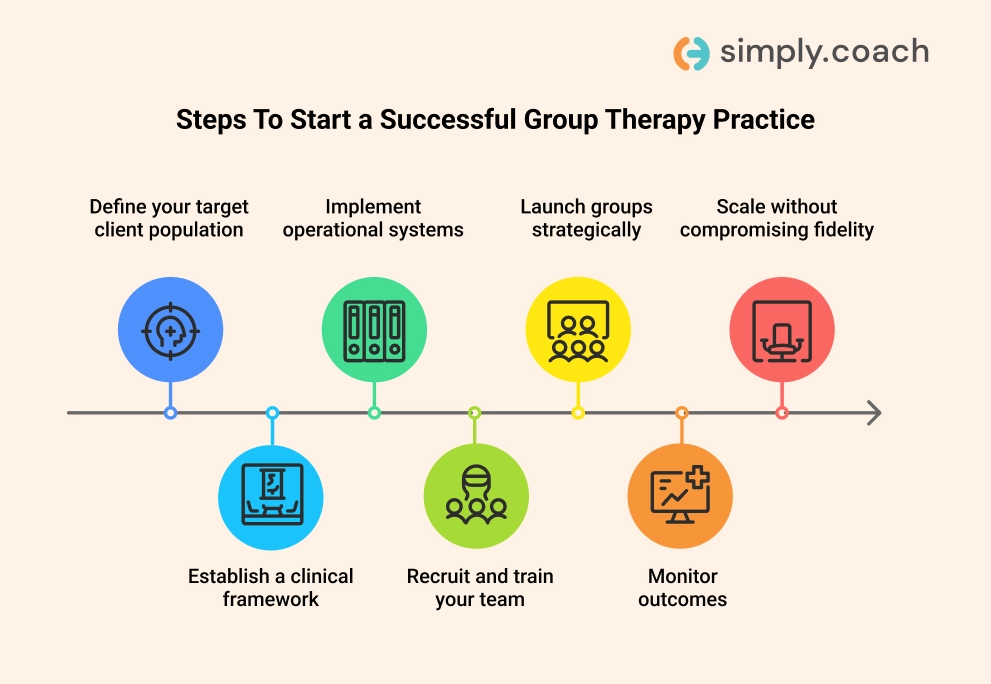
Step 1: Define your target client population
Choosing the right client population is foundational for successful group therapy. Cohesion, safety, and therapeutic impact depend on how well participants match each other in clinical presentation and readiness. You need to consider diagnosis, emotional regulation capacity, trauma history, and relational functioning to optimize outcomes.
- Identify clients whose presenting issues align with your chosen modalities, e.g., DBT for emotion dysregulation or ACT for experiential avoidance.
- Screen participants for trauma severity, comorbidities, or instability that might necessitate individual therapy first.
- Limit group size based on modality and intervention intensity: 6–10 for interpersonal learning groups, 12–15 for psychoeducational interventions.
- Match participants by therapy experience, coping skills, and functional readiness to prevent group destabilization.
Step 2: Establish a clinical framework
A structured framework ensures your sessions are predictable, safe, and evidence-based while allowing flexibility for individual and group needs. Define session phases, facilitation protocols, and therapeutic techniques to maintain both fidelity and efficacy.
- Map out the five stages of group therapy: orientation, working, insight/catharsis, problem-solving/social learning, and termination.
- Integrate modality-specific techniques, psychodrama, IPT, DBT, ACT, or mindful self-compassion exercises into session flow.
- Assign co-facilitators specific roles for observation, relational feedback, and risk management.
- Establish measurable clinical outcomes such as interpersonal skill development, relational insight, and emotional regulation improvements.
Step 3: Implement operational systems
Operational systems prevent administrative tasks from interfering with clinical work and ensure smooth session flow. Automating and structuring processes keeps clients engaged and allows you to maintain high-quality facilitation without burnout.
- Use centralized client workspaces for session notes, goal tracking, and progress dashboards.
- Automate pre-session forms, homework, and behavioral nudges to reinforce therapeutic engagement.
- Incorporate HIPAA-compliant video conferencing, secure file sharing, and remote session management for hybrid groups.
- Standardize outcome tracking, attendance monitoring, and supervision logs to maintain clinical oversight and compliance.
Step 4: Recruit and train your team
Your co-facilitators’ skillset directly impacts client safety, group cohesion, and treatment outcomes. Recruiting therapists with expertise in your modalities and providing structured training ensures consistent therapeutic delivery.
- Assess co-therapists’ mastery in DBT, ACT, IPT, psychodrama, or mindful self-compassion approaches.
- Implement post-session debriefing and reflective supervision protocols to maintain clinical fidelity.
- Train clinicians in rupture repair, early de-escalation, and high-risk intervention management.
- Decide on employment type (IC vs. W2) considering supervision needs, insurance coverage, and legal compliance.
Step 5: Launch groups strategically
Launching your first group requires aligning clinical readiness with operational execution. Orientation, safety protocols, and initial cohort composition set the tone for engagement and therapeutic depth.
- Conduct orientation sessions to explain rules, confidentiality, commitment expectations, and safety procedures.
- Recruit participants through professional referrals, targeted outreach, and existing client networks.
- Pilot small groups to refine facilitation flow, modality application, and relational dynamics.
- Highlight expected outcomes, emotional regulation, interpersonal insight, and behavioral skill development during recruitment.
Step 6: Monitor outcomes and optimize processes
Continuous monitoring allows you to identify gaps in both clinical and operational processes and make timely adjustments. Use data-driven approaches to maintain efficacy while enhancing client engagement.
- Track standardized clinical measures such as symptom reduction, skill acquisition, and interpersonal functioning.
- Collect structured participant feedback on engagement, group cohesion, and facilitator effectiveness.
- Adjust session structure, group composition, or facilitation strategies based on observed outcomes.
- Audit administrative processes: no-show trends, homework adherence, documentation quality, and goal completion.
Step 7: Scale without compromising clinical fidelity
Scaling your practice requires careful expansion to preserve therapeutic quality across multiple groups. A systematic approach allows you to grow while maintaining safe, structured, and effective group interventions.
- Introduce new cohorts gradually, staggering modality-specific groups (DBT, ACT, IPT) to manage complexity.
- Maintain centralized tracking for client progress, session outcomes, and therapeutic observations across all groups.
- Expand the co-facilitator team with structured supervision to ensure consistent standards.
- Routinely evaluate group outcomes and session fidelity to ensure clinical rigor remains uncompromised.
With a plan in place, practical pre-launch tips help ensure your first sessions run smoothly.
7 Mistakes to Avoid When Starting a Group Therapy Practice
Operational missteps, clinician misalignment, or poorly defined clinical protocols can directly affect client safety, therapeutic efficacy, and group cohesion. Recognizing these risks before you launch protects outcomes and practice sustainability.
- Scaling before testing protocols
Launching multiple groups without piloting intake procedures, group norms, and session structure often leads to uneven client engagement and premature dropouts. Always pilot a single cohort first to monitor engagement, emotional regulation, and group cohesion.
- Lacking documented clinical procedures
Not creating structured SOPs for intake screening, crisis management, no-show policies, or termination protocols increases the risk of liability and inconsistent care. Document every step, from pre-group assessment to post-session follow-up.
- Misaligning clinician competencies
Hiring clinicians without evaluating alignment in modality, population expertise, or co-facilitation skills can destabilize group dynamics. Match clinicians to the therapeutic model and establish clear supervision protocols for interventions.
- Neglecting administrative infrastructure
Skipping HIPAA-compliant notes, automated reminders, scheduling systems, or facilitating payments results in missed sessions, lost revenue, and clinician burnout. Integrate a unified platform for documentation, session tracking, and client engagement.
- Underestimating financial and regulatory demands
Failing to budget for clinician compensation, professional liability insurance, training, or licensing compliance can derail operations. Plan for overhead, malpractice coverage, and state-specific group therapy regulations.
- Undefined target client criteria
Admitting clients without precise inclusion/exclusion criteria undermines group safety and therapeutic outcomes. Consider trauma history, emotional regulation capacity, co-morbidities, and readiness for group disclosure before enrollment.
- Skipping ongoing supervision and structured consultation
Not scheduling regular case reviews, co-facilitator debriefs, or advanced clinical supervision risks clinician drift and ethical oversights. Implement structured supervision to monitor transference, countertransference, and group process dynamics.
Now that you understand potential pitfalls, Simply.Coach can help manage operations with session scheduling, progress tracking, and workflow management for effective group therapy.
Take Command of Your Group Therapy Practice with Simply.Coach

Managing a group therapy practice means coordinating participant screening, co-facilitator schedules, session logistics, and detailed clinical documentation, without compromising therapeutic integrity. Simply.Coach centralizes these operations, allowing you to track client progress, maintain treatment fidelity, and oversee multiple cohorts efficiently.
- Goal & development planning: Set structured objectives for individuals and groups, assign action items between sessions, and track measurable progress for each client.
- Team engagement: Coordinate co-facilitators, align on session plans, and track group dynamics collaboratively to maintain consistency across all group sessions
- Action plans: Organize participant assignments, skills practice, and follow-up tasks to reinforce in-session interventions and maximize skill generalization.
- Notes: Capture co-facilitator observations, session dynamics, and individual responses in a centralized, secure platform to support case formulation and supervision.
- Client workspaces: Provide participants with controlled access to group session materials, exercises, and psychoeducational content while maintaining confidentiality and structured engagement.
- Scheduling: Coordinate multiple groups and co-facilitators, integrate calendars, and allow clients to self-book sessions within your approved availability, reducing no-shows.
- Reports: Generate detailed client- and group-level progress reports, providing actionable insights to refine interventions and support clinical decision-making.
With Simply.Coach, you can structure and scale your group therapy practice with precision, tracking participant outcomes, coordinating co-facilitators, managing session materials, and ensuring every client receives consistent, evidence-based care.
Conclusion
Launching a group therapy practice requires more than assembling a room of clients; it demands deliberate clinical design, structured session frameworks, and careful management of group dynamics. From defining your target population to selecting evidence-based modalities like DBT, ACT, or mindful self-compassion, each decision impacts therapeutic outcomes and client engagement.
Implementing SOPs, choosing the right clinicians, managing scheduling, and establishing reporting mechanisms prevent clinical drift, reduce no-shows, and maintain treatment fidelity. These foundational systems allow you to focus on delivering interventions while sustaining a high-functioning practice without compromising care quality.
If you want to scale their group practice without losing control over therapeutic quality,Simply.Coach, through their all-in-one HIPAA-compliant therapy practice management software, helps integrate these clinical and operational needs seamlessly. With tools like prospect management, action plans, scheduling, and team engagements, you can track participant progress, coordinate co-facilitators, and manage multiple therapy cohorts while preserving clinical rigor.
FAQs
1. What is the ideal group size for effective therapy?
Group size typically ranges from 6 to 12 participants, balancing enough diversity for interpersonal learning with sufficient intimacy for trust and vulnerability.
2. How do I select participants to ensure group cohesion?
Screening should assess symptom severity, motivation, interpersonal functioning, and potential triggers, ensuring the group can safely engage in mutual exploration without destabilizing dynamics.
3. Can I run multiple modalities within one group practice?
Yes, but each group should maintain a consistent theoretical framework (e.g., DBT or ACT) per cohort to avoid clinical drift and confusion among participants.
4. How do I handle no-shows in group therapy?
Automated reminders, pre-session forms, and clear attendance policies help reduce no-shows while maintaining accountability and preserving the therapeutic flow for the entire group.
5. Should I accept insurance for group sessions?
If you do, ensure your billing codes align with group therapy standards, and clarify coverage limits upfront to avoid client misunderstandings or delayed reimbursements.
6. How can co-facilitators be effectively integrated?
Clearly define roles, session responsibilities, and communication protocols; regular supervision and reflective practice ensure alignment and consistent therapeutic interventions.
7. What legal or ethical considerations should I keep in mind?
Obtain informed consent, maintain confidentiality within group limits, screen for risk factors, and implement crisis protocols to ensure both ethical and clinical compliance.
About Simply.Coach
Simply.Coach is an enterprise-grade coaching software designed to be used by individual coaches and coaching businesses. Trusted by ICF-accredited and EMCC-credentialed coaches worldwide, Simply.Coach is on a mission to elevate the experience and process of coaching with technology-led tools and solutions.
