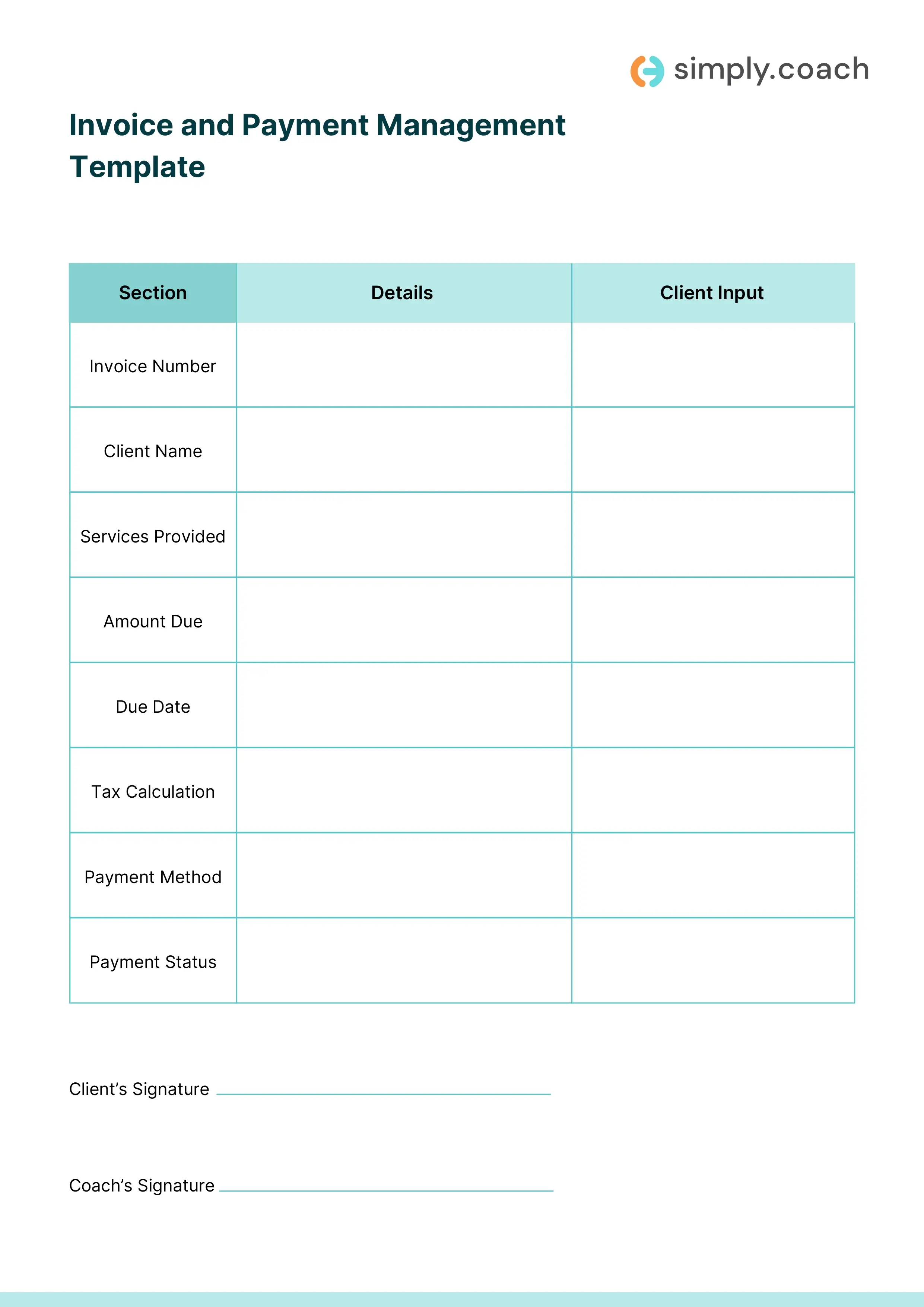
This SOAP Notes Template helps therapists and counselors capture symptoms, findings, assessments, and treatment plans in a clear, structured format.

SOAP Notes Template
What Is the SOAP Notes Template?
The SOAP Notes Template is a standardized documentation tool widely used in healthcare, counseling, and therapy. SOAP stands for Subjective, Objective, Assessment, and Plan,the four essential sections that provide a clear snapshot of each session. This format supports clinical accuracy, treatment continuity, and professional compliance.
How to Use This Template


Subjective
Record client-reported symptoms and personal concerns.
Objective
Note measurable or observable findings, such as physical or behavioral signs.
Assessment
Document your professional evaluation of the client’s condition or progress.
Plan
Outline next steps, treatment recommendations, or follow-up actions.


Why Professionals Use This Template
Ensures consistent documentation
across sessions
Supports accurate treatment planning
and client care
Widely recognized and accepted
across healthcare and counseling practices
How Therapists & Clinicians Use This Template
To streamline documentation
Emily, a clinical psychologist, uses SOAP notes after every session to keep her records organized and compliant.
To monitor progress over time
James, a counselor, reviews past SOAP entries to identify recurring themes and track improvements.
To collaborate with other professionals
Rachel, a psychiatrist, shares structured SOAP notes with medical teams for coordinated care.
Frequently Asked Questions
Is this template only for medical professionals? −
Not at all. SOAP notes can be used by therapists, counselors, coaches, and healthcare providers alike.
Can I adapt this format to my practice? +
Yes, the template is fully editable, so you can customize language or sections as needed.
Does this work for both digital and paper notes? +
Yes, you can fill it out electronically or print it for handwritten use






